BioWire Bytes 011 – Living Near Golf Courses Tied to Higher Parkinson’s Risk
Byte-sized biotech
Researchers flagged an seemingly innocuous neighborhood risk for Parkinson’s disease: living close to a golf course. Why might this be? It turns out those manicured fairways and putting greens may hide a hazard beyond the occasional stray golf balls — the chemicals that are sprayed on them. A study reported that people residing near pesticide-treated golf courses have higher odds of developing Parkinson’s disease (PD), giving evidence to the long-suspected link between pesticides and and at least one neurodegenerative illness.
First, if you enjoy these updates, consider subscribing and becoming a part of our growing community!
Parkinson’s disease is the world’s fastest-growing brain disorder, and scientists have long suspected that environmental exposures play a big part. Decades of research have linked pesticide exposure, from farm insecticides to weed killers, with elevated PD risk, e.g., farmers and others with heavy pesticide contact tend to develop Parkinson’s at higher rates (Tanner et al., 2011). The logic is simple if a bit unsettling, chemicals potent enough to kill insects and weeds might also harm human brain cells over time. Until now, however, one everyday source of pesticide exposure remained under the radar, golf courses. In the United States, golf courses are doused with pesticides to keep them lush and green, in fact, American courses use up to 15 times more pesticides than their European counterparts. Given that many golf courses sit near residential neighborhoods, the question practically asked itself:
Can all those chemicals be seeping into the environment and contributing to Parkinson’s disease in nearby residents?
New Evidence from the Midwest Study
To find out, researchers dug into decades of health data from 27 counties in Minnesota and Wisconsin between 1991 and 2015 (Krzyzanowski et a., 2025). They identified 419 people who developed Parkinson’s disease (and matched them with over 5,000 similar individuals who did not have PD) to see if living near golf courses was more common among the PD group. What they found was eye-opening:
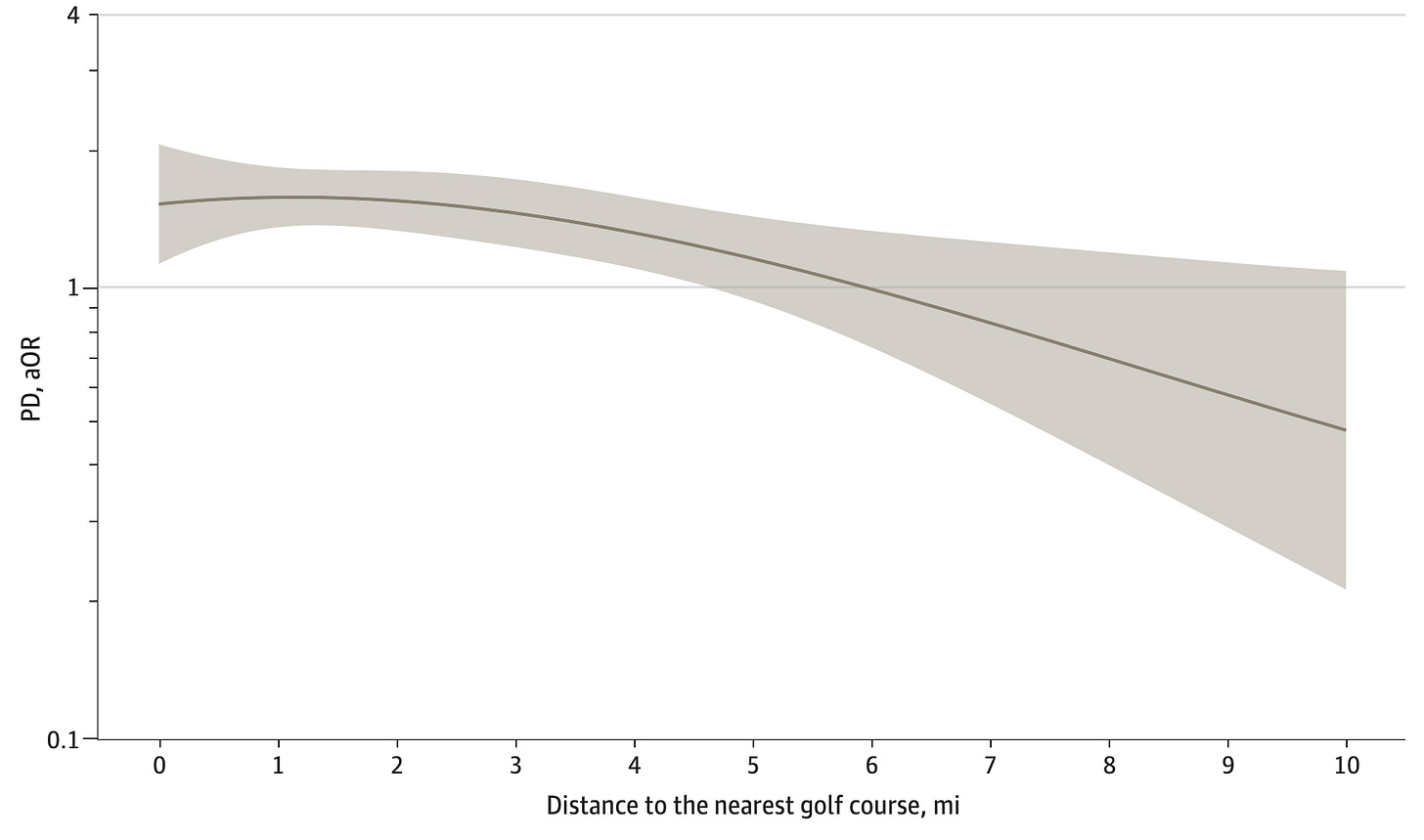
Distance mattered. Living very close to a golf course was associated with a significant jump in Parkinson’s risk. Individuals who lived within one mile of a golf course were more than twice as likely to develop PD as those who lived over six miles away. In fact, the data showed a dose-dependent pattern, people within roughly a 1–3 mile radius of a course had elevated PD odds, and the risk peaked up to about 3 miles out. Beyond three miles, the threat appeared to taper off, each additional mile away from the course was linked with a notable decrease in risk. In other words, the farther you lived from the greens, the safer you were.
Water was a conduit. The study also found nearly double the odds of Parkinson’s among residents whose homes were supplied by water systems that include a golf course, compared to those whose water source had no golf course in the mix. The risk was highest of all when the golf course sat on vulnerable groundwater, areas with porous soil or shallow aquifers where pesticides could easily leach into drinking water. In those situations, Parkinson’s risk climbed even further. These findings point to contaminated water and possibly airborne drift of chemicals as likely routes of exposure linking golf course pesticides to people’s bodies.
Notably, within that first 1–3 mile range, being even closer than a mile didn’t significantly increase risk beyond the already elevated level, suggesting there might be a saturation point or “ceiling effect” to the exposure. But the overall trend was clear, proximity to pesticide-heavy golf courses correlated with higher Parkinson’s disease rates in this large population-based analysis, even after accounting for age, sex, income, and whether the area was urban or rural.
Rethinking Pesticide Use in Our Backyards
Before you panic about the golf course down the street, it’s important to emphasize that this study shows association, not outright proof of causation. Living near a golf course doesn’t guarantee someone will develop Parkinson’s, and many other factors (from genetics to other pollutants) contribute to the disease. The researchers themselves caution that they used residential distance and water source as indirect measures of pesticide exposure – they didn’t directly measure chemicals in people’s bodies. And yet, the results align strikingly with what we already know about Parkinson’s and toxins. It’s a strong signal that something environmental is at play here, likely the intense pesticide use on courses.
The implications are both concerning and cautiously optimistic. On one hand, the idea that a pleasant golf green in your community might quietly raise your risk of a serious brain disease is unsettling. It underscores how our land-use choices – like maintaining perfect lawns with heavy chemical use – can have hidden health costs. On the other hand, if pesticide exposure is indeed a key factor in Parkinson’s disease, that’s actually actionable knowledge. Unlike age or genetics, pesticide use is something we can change. Communities and regulators could take steps to curtail high-risk pesticide practices: for example, adopting more eco-friendly turf management on golf courses, buffering residential areas from pesticide drift, or protecting vulnerable groundwater zones from contamination.
Parkinson’s disease currently has no cure, so prevention is all we really have. Hopefully, this study can serve as a wake-up call that the environment where we live and play matters for our neurological health. While more are needed (and are surely underway) to confirm these findings in other regions and nail down the exact mechanisms, the clear takeaway is that there are likely neurological consequences to chronic pesticide exposure. Reducing heavy pesticide use, especially in places entwined with our water supplies and neighborhoods, would be a smart move and general public service to help protect the brain health in our communities.
These newsletters take significant effort to put together and are totally for the reader's benefit. If you find these explorations valuable, there are multiple ways to show your support:
Engage: Like or comment on posts to join the conversation.
Subscribe: Never miss an update by subscribing to the Substack.
Share: Help spread the word by sharing posts with friends directly or on social media.
References:
Krzyzanowski, B., Mullan, A.F., Dorsey, E.R., Chirag, S.S., Turcano, P., Camerucci, E., Bower, J.H. and Savica, R., 2025. Proximity to Golf Courses and Risk of Parkinson Disease. JAMA Network Open, 8(5), pp.e259198-e259198.
Tanner, C.M., Kamel, F., Ross, G.W., Hoppin, J.A., Goldman, S.M., Korell, M., Marras, C., Bhudhikanok, G.S., Kasten, M., Chade, A.R. and Comyns, K., 2011. Rotenone, paraquat, and Parkinson’s disease. Environmental health perspectives, 119(6), pp.866-872.



I have become so suspicious of tap water, I exclusively get well water filled in a 5-gallon container sent to me each week.
reminder that we are part of a (eco)system: everything flows back and forth